Definition of an Ulcer: an open sore on an external or internal surface of the body, caused by a break in the skin or mucous membrane that fails to heal.
Medical wound care: steps taken to ensure that a wound such as a foot ulcer heals correctly
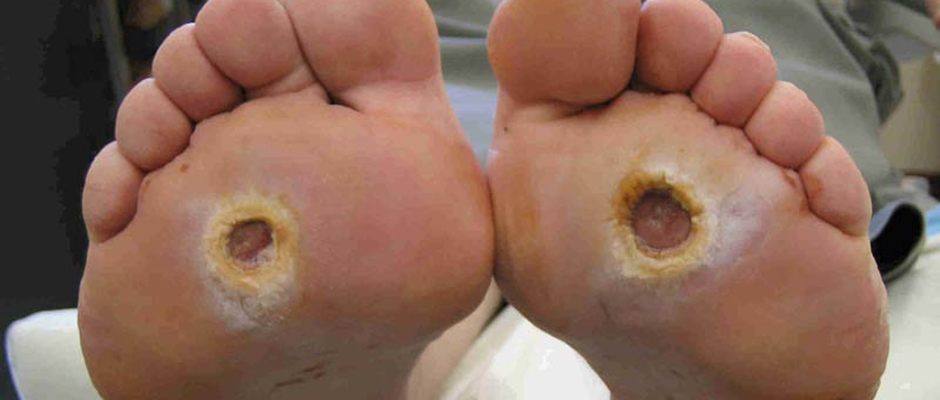
An ulcer is an open wound in the skin that appears as an open crater and exposes the deeper tissue. Ulcers are wounds that generally will not heal or keep reoccurring.
What does an ulcer look like?
[list style=”arrow” color=”blue”]
- Open sore exposing deeper tissue
- Skin around sore may be red, swollen and painful
- Fluid may ooze from the ulcer (blood or pus)
- May have a swollen leg with burning or itching sensations
[/list]
Common Ulcers of the Leg and Foot
Common ulcers of the leg and feet are Venous ulcers, Arterial ulcers (ischemic ulcers), and Neuropathic ulcers. Click below to learn more about each type.
[reveal title=”What are Veneous Ulcers” open=”false” color=”blue”]Venous ulcers are commonly seen above the calf or on the lower ankle. Venous ulcers are most common in patients who have a history of swollen legs, varicose veins or a history of blood clots.
Characteristics of a venous ulcer are:
A shallow sore, sometimes of irregular shape that appears on the lower leg or ankle, often associated with contact dermatitis. Venous ulcer may or may not be painful.
Risk factors for a venous ulcer are:
Deep vein thrombosis (blood clot), Congestive heart failure, Varicose veins, pbesity, long periods of sitting or bed rest and pregnancy.[/reveal][reveal title=”What are Arterial Ulcers?” open=”false” color=”blue”]Arterial ulcers are commonly seen on the outside (lateral) part of the foot, ankle or leg. Arterial ulcers are most common in patients with very poor circulation and blood flow to the leg. When pressure is placed on the skin, due to foot structure or even ill-fitting footwear, the skin is damaged but unable to repair itself due to poor blood flow to the tissue, which can lead to an ulcer.
Characteristics of an arterial ulcer:
Arterial ulcers are typically deep and sore with a punched out appearance with smooth edges around the wound. Arterial ulcers are found mainly on the outside (lateral) of the leg or foot. Wounds result in skin is pale, shiny, thin and taut, very tender and painful, however there is often minimal to no drainage from the wound.
Risks for an arterial ulcer are:
Increased risk for an arterial ulcer comes when a patient as one of more of to following conditions: poor circulation, renal disease, increased aged, certain disease such as diabetes or peripheral arterial disease, and ill-fitting footwear can increase your risk.[/reveal][reveal title=”What are Neuropathic Ulcers?” open=”false” color=”blue”]Neuropathic ulcers are associated with patients who have lost their sensation to pain. Patients will typically exert a lot of pressure at certain spots under their feet when they walk creating a build-up of callus. As time progresses, the pressure becomes so high that the callused area eventually breaks down and an ulcer is formed except the patient will hardly notice any pain.
Characteristics of a Neuropathic ulcer are:
Neuropathic ulcers are located typically around the bottom of the foot or the tips of toes, are painless and are usually surround by callus (thick, dead skin).
Risks for a neuropathic ulcer are:
One is a greater risk for Neuropathic ulcers if one has a history of foot ulcers, loss of sensation in the feet (neuropathy),
poor circulation, swollen feet, or wears ill-fitting footwear.[/reveal][divider_line type=”divider_line”]
How can ulcers be prevented?
By decreasing the major risks of ulcers you can help prevent ulcers from developing or getting worse. Things you can do to prevent ulcers are:
[list style=”arrow” color=”blue”]
- Quit smoking
- Control your cholesterol levels
- Manage your blood pressure
- Manage your diabetes and control your blood sugar levels
- Discuss possible drug therapies with your family physician to prevent blood clots
- Exercise (seek medical advice from your family physician before starting)
- See your family physician at least once a year for a full physical examination
- See your foot specialist to get a comprehensive foot exam performed
[/list]

